Types of Lower Back Pain
Hip pain, sciatica, lumbar, trigger point, numbness, tingling, sacroiliac, bursa, bursitis, disc, disc degeneration protruding disc, herniated disc, pinched nerve, spinal nerve, nerve root, back pain, paralytic ileus, irritable bowel syndrome, constipation, sexual dysfunction, dysmenorrhea

Symptoms of lower back pain can range from mild to incapacitating, occasional to constant, and local to radiating.
It is common to feel lower back pain being referred downward into one or both hips and one or both legs. Although pain being generated from the disc is by far the most common cause, other structures can also cause back pain and refer pain into the hips and legs including joints, muscles or fascia (connective tissue), and organs.
Back pain and joint dysfunction can also cause problems with organ function such as paralytic ileus, irritable bowel syndrome, constipation, sexual dysfunction, and dysmenorrhea. This is due to the intimate connection of the spine and the nervous system through visersomatic reflexes.
Many people are mistakenly diagnosed with “Sciatica” because an individual is experiencing hip or leg pain associated with lower back pain.
We must always remember that the source of the pain (pain generator) is not synonymous with the cause of the pain. A common example of a pain generator in the case of lower back and leg pain is the spinal disc. Either something has caused an acute injury to that structure or the structure is under enough stressful load to make pain receptors within it light up. In most cases, the cause of the issue was a combination of joint dysfunction, muscle imbalance, poor muscular stability, and poor ergonomic habits that lead to a repetitive stress /strain injury over a period of time. Because of the complex nature of these problems, focusing on a singular assessment or treatment approach to address these issues is unwise, especially in recurrent and chronic cases.
Sitting – There is no position that creates more pressure in the spinal discs than sitting. It is critical that we sit with proper lumbar support to maintain the curvature of the lower back. Proper posture minimizes the damaging effects of prolonged sitting. Sitting improperly will undoubtedly contribute to lumbar disc degeneration.
Lifting – It is of the utmost importance that you lift properly. This involves having the object close to your center of gravity, keeping your lower back erect before and during the lift, and lifting with your legs. Of equal importance is placing the object down carefully. The majority of injuries occur when people are setting down the object they had lifted. You must apply the same rules to setting something down as when lifting something up, just in reverse order.
Twisting – Did you know that the professional sport with the highest rate of chronic lower back pain was golf? Vacuuming and mopping are very difficult for people with lower back trouble. Repetitive twisting can cause a problem, especially under any type of load. When lifting, always keep your spine in a straight and neutral position. Turn your whole body. Don’t just twist.
Lower Back Pain Sources
There are many causes of lower back and leg pain, which can create a similar clinical picture.
The disc is the most common source of lower back and leg pain. However, there are usually several different components that lead to the injury and the pain being generated.
Damaged Disc
Due to repetitive stresses or sudden trauma, the gel in the center of the disc can tear into the rings of ligament surrounding it. That tear becomes a weak spot in the disc that is more likely to become reinjured in the future. When the closer rings surrounding the gel are torn, local lower back pain is produced. As the tear progresses radially outward, the pain moves further into the hip and leg. This is commonly misdiagnosed as sciatia. The accurate diagnosis would be Internal Disc Derangement because the entire injury is contained within the disc.
Sciatica
Sciatica is caused when the spinal nerve exiting at the affected level is irritated or compressed. This occurs when the radial tear either begins to significantly deform the outer disc putting pressure on the nerve, or ruptures through the outer disc, compressing the adjacent spinal nerve.
Joint Pain
Lumbar facet joints, the sacroiliac joints, and the hip joints can create local or referred pain patterns. Specific diagnosis is made by performing a detailed history, examination, and analyzing regional imaging. This diagnosis dictates the treatment approach, which can vary greatly depending on the cause. Below is a typical pain referral pattern related to the sacroiliac joint:
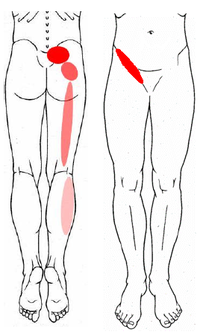
Muscular Trigger Points
According to the Academy of American Family Physicians, “Trigger points are discrete, focal, hyperirritable spots located in a taut band of skeletal muscle. They produce pain locally and/or in a referred pattern and often accompany chronic musculoskeletal disorders.” They go on to say, “These include muscles used to maintain body posture, such as those in the neck, shoulders, and pelvic girdle. Trigger points may also manifest as tension headache, tinnitus, temporomandibular joint pain, decreased range of motion in the legs, and low back pain.”
Determining if an individual’s pain is caused by trigger points can be very tricky. It is essential that the clinician have a detailed knowledge of all of the potential pain referral patterns. The example below of a trigger point in the gluteal medius muscle is commonly misdiagnosed as Sciatica involving the spinal nerve.

Organ Disease
Clinicians must consider non-musculoskeletal sources in their list of possible diagnoses when evaluating their patients. Some examples of these include:
- Kidney disease – Lower back pain
- Abdominal Aortic Aneurysm – Lower back pain
- Disease of the reproductive organs – Lower back or hip pain
- Vascular disease – Leg pain
Solution to Lower Back Pain
These problems are shown to often times have many contributing factors.
These factors include such issues as spinal joint dysfunction (malfunctioning of the spinal joints), muscle imbalances, weakness of the supporting spinal musculature (Deconditioning Syndrome), improper movement patterns, poor posture/ergonomic habits, and chronic inflammation.
Because these problems tend to be complex, and the rate of disability is significant, a multi-specialty team approach is best.
At Palmetto Physical Medicine, not only are the specialists each doing what they are best at doing, but they are working together to provide the optimum benefit for the patient.
The primary goal initially is to return the individual to function as quickly as possible. This is followed up with patient education on spinal strengthening and physical fitness, skill training, and ergonomic modification to best prevent recurrences.
This approach has shown quicker recovery times, faster return to work, decreased re-injury rates, and less therapist dependence.
Call Palmetto Physical Medicine today at 864-437-8930 to schedule an appointment.
